Clinical
Case Report
Quantifying Muscle Compressibility as a New Decision Support
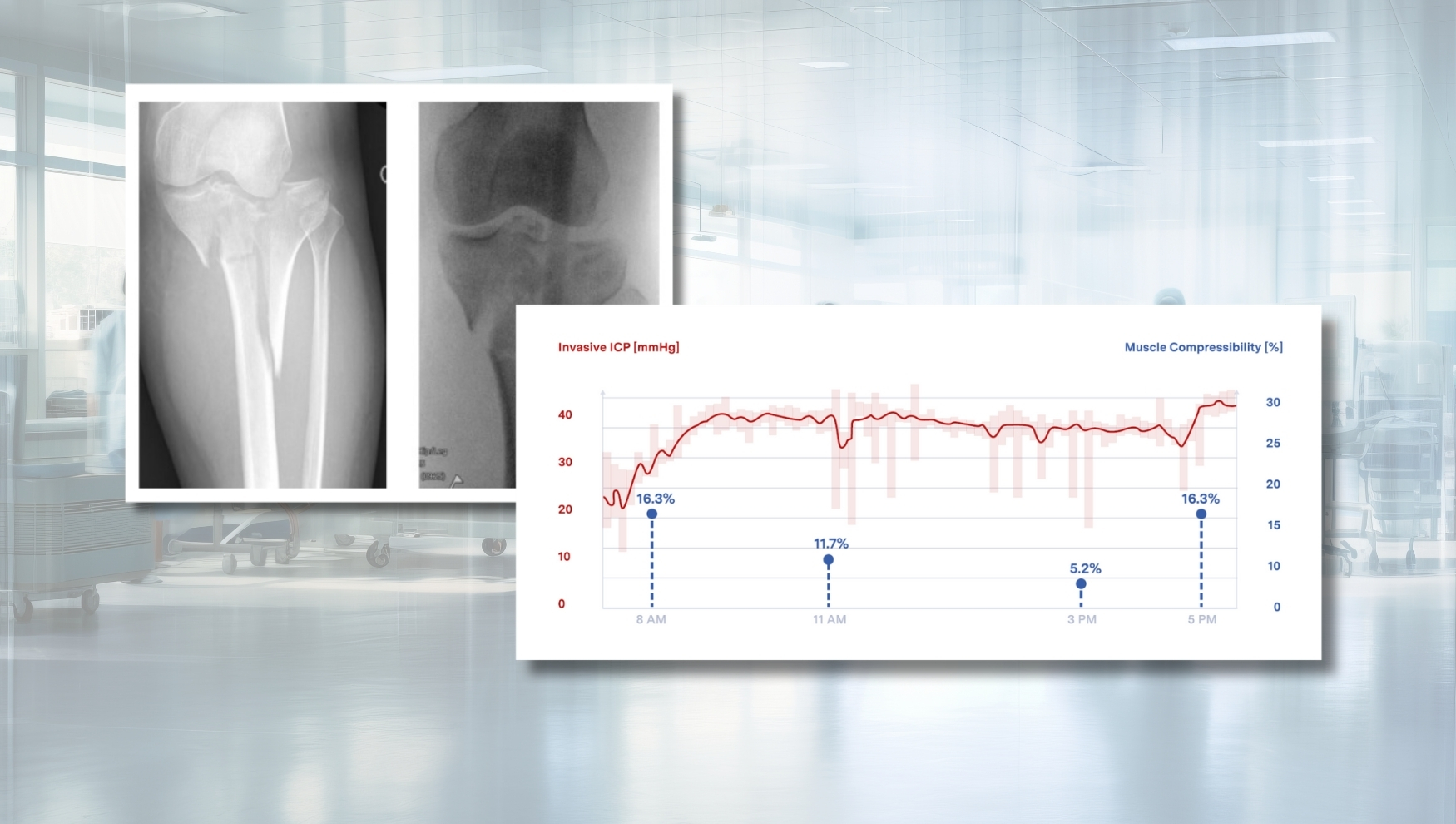
When pressure readings and clinical signs diverge.
Objective
Introduction
Traditional criteria for diagnosing compartment syndrome have shown limited reliability. Pressure thresholds, single-point measurements, and the classic “P” signs have high variability and correlate poorly with tissue ischemia. These findings suggest the invasive gold standard may not accurately reflect tissue health, motivating the exploration of non-invasive, quantifiable methods for soft tissue assessment.
Solution
Case Presentation
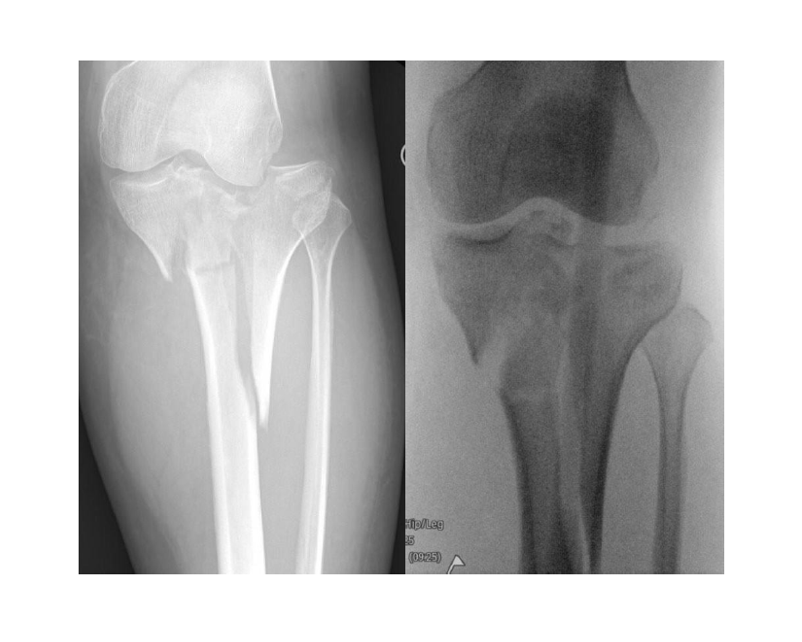
A 40-year-old female sustained a displaced tibial plateau fracture (fig.1) with marked soft-tissue swelling, tibia offset and joint depression, conferring ~50% ACS risk.
Temporary stabilization was achieved using an external fixator.
Continuous Invasive Intracompartmental Pressure (ICP) monitoring was initiated.
Result
ICP Trend
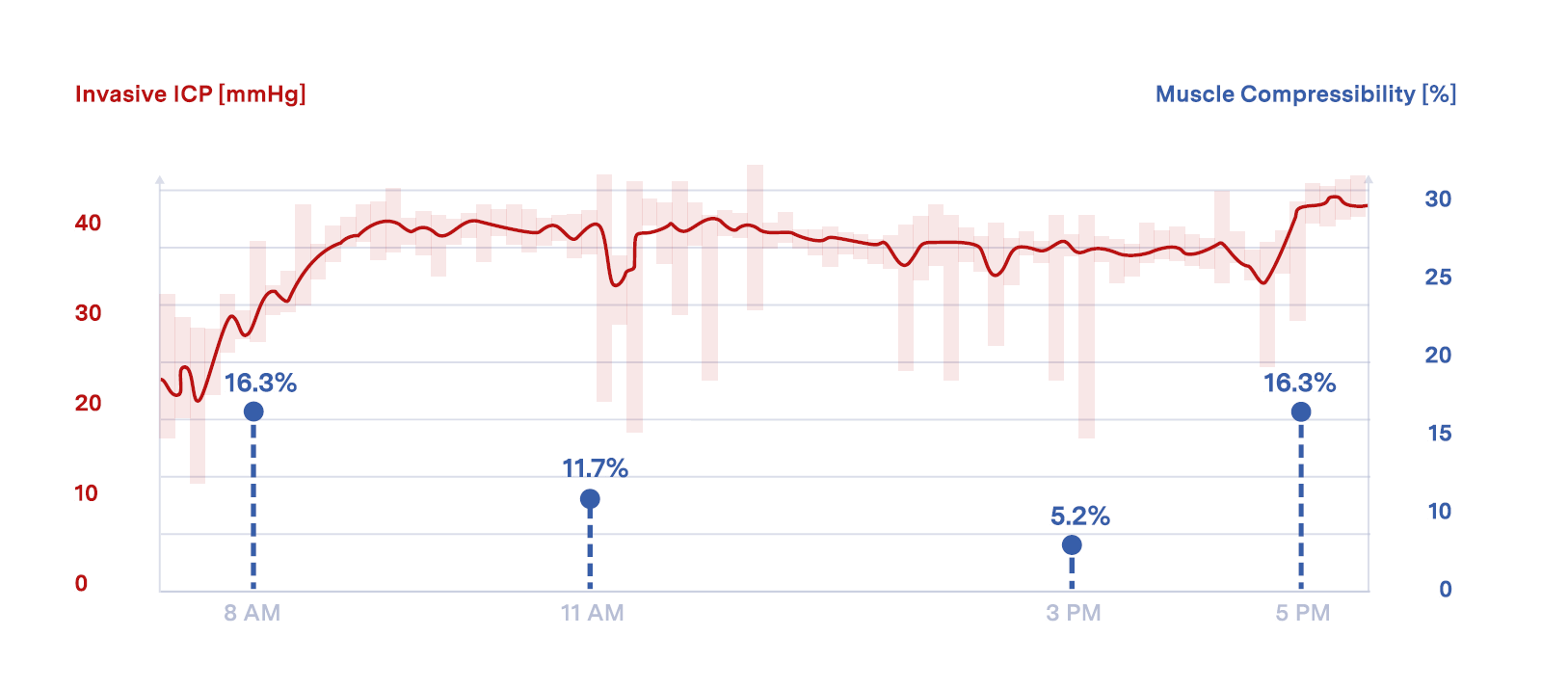
When the catheter was inserted, the pressure was 30 mmHg and rose to 45 mmHg within 2 hours. It remained elevated for ~20 hours.
Clinical Status
The patient showed no progressive pain, neurological deficit, or tense compartment.
Quantis ST Measurements
Non-invasive soft tissue compressibility measurements were performed using the Compremium Quantis ST device in the anterior compartment of the left lower leg. Compartment compressibility (CP Value) is the percentage change in compartment thickness between low and high applied pressures.
Compressibility values dropped from 16.3% to 5.2% within 6 hours, followed by a recovery to the baseline of 16.3% after ~2 hours.
Outcome and conclusion
ICP remained high and stable, showing poor correlation with clinical findings, suggesting prophylactic fasciotomy. In contrast, compressibility measurements declined but rebounded to baseline, aligning with clinical and patient outcomes. No fasciotomy was therefore performed.
The patient achieved full functional recovery without complications.
This case was presented at OTA 2025 by Andrew H. Schmidt, MD Chief Orthopedic Surgery Hennepin Healthcare Minneapolis, MN, USA




