Why This Innovation Exists
Making venous pressure a measurable, actionable signal
Venous pressure plays a critical role in patient deterioration across acute and chronic disease.
Elevated venous pressure contributes to:
- venous congestion
- organ dysfunction in critical illness
- decompensation in heart failure
- challenges in fluid management across dialysis and vascular care.
Clinicians have long understood the importance of venous physiology. Venous pressure holds essential information about circulatory status and disease progression.
The problem was never clinical relevance.
The problem was access.
The problem was access.
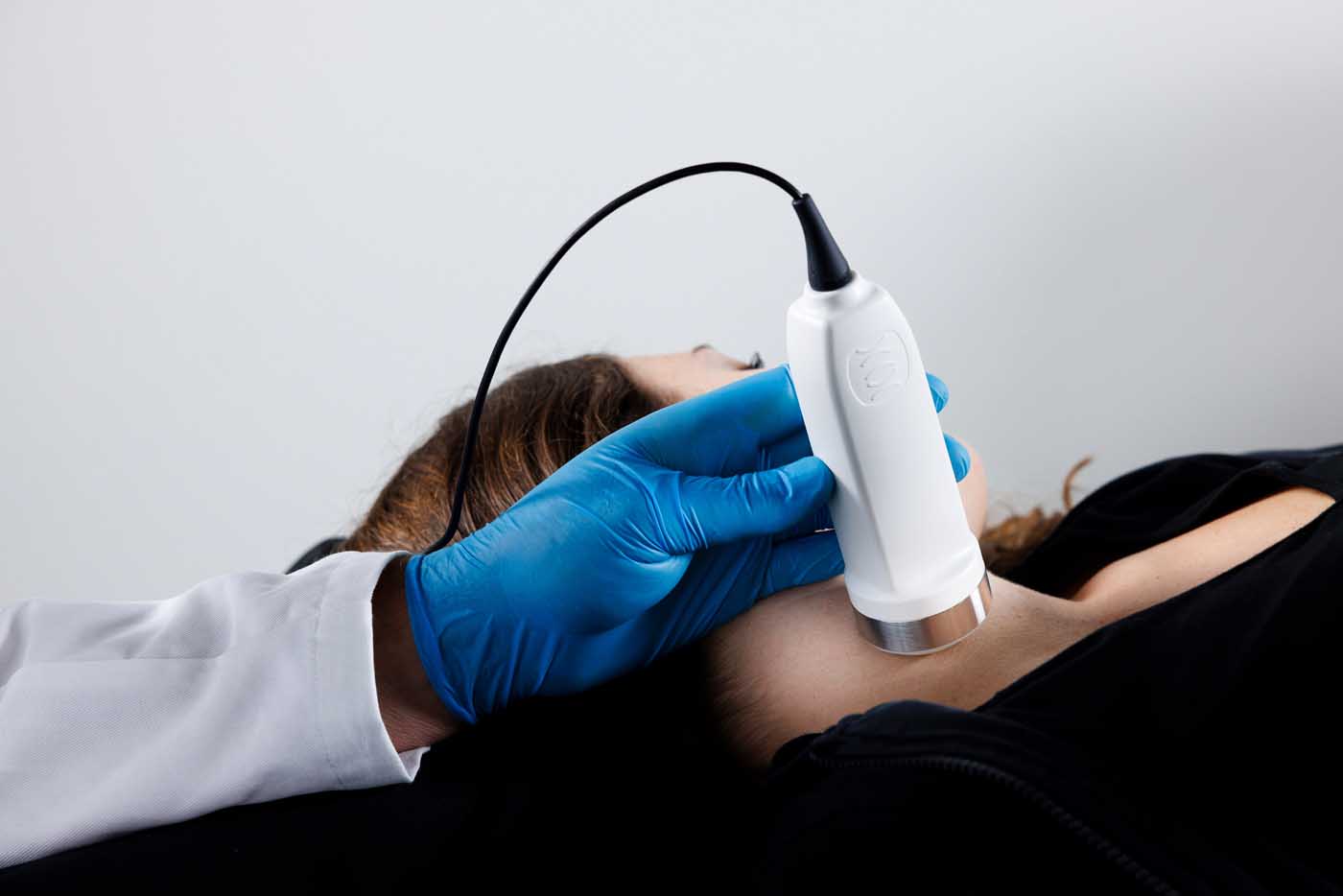


The long-standing limitation
Central Venous Pressure (CVP) was one of the earliest attempts to make venous pressure measurable.
It mattered because it reflected something fundamental about circulatory physiology.
It mattered because it reflected something fundamental about circulatory physiology.
But meaningful measurement came with significant constraints.
- Accurate CVP assessment required invasive central venous catheterisation
- Clinical estimation proved unreliable and inconsistent
- Existing non-invasive surrogates lacked quantitative repeatability
As a result, venous pressure remained clinically important, but difficult to assess safely, consistently, and beyond highly controlled settings.
The persistent gap
Across emergency departments, hospital wards, outpatient clinics, and dialysis centers,
clinicians make critical decisions every day with limited objective insight into venous pressure
and its contribution to venous congestion.
clinicians make critical decisions every day with limited objective insight into venous pressure
and its contribution to venous congestion.
This is not a failure of understanding.
It is a limitation of the standard of care.





